Lipedema: symptoms and treatments
Lipoedema or ”large leg syndrome” is a chronic progressive disorder of the adipose tissue with a lymphatic component. Affecting mainly women – about 11% of them to varying degrees – it considerably affects their quality of life.
Let’s have an update on this disorder and its treatment.
Lipedema is characterized by an abnormal, bilateral and symmetrical distribution of subcutaneous fatty tissue of the lower limbs or, very rarely, of the upper limbs, associated with a moderate edema. It causes spontaneous pain when pressed or pinched, a feeling of skin tension and frequent bruising.
Often confused with obesity, lipodystrophy or lymphedema, it remains unfortunately relatively unknown to both the medical profession and the general public.
However, it has a strong impact on patients’ body image and quality of life.
Origins of lipedema
Lipedema is a condition that is most likely hereditary in origin (1) and related to periods of hormonal changes such as puberty, pregnancy or menopause. It usually starts progressively from adolescence onwards, then evolves more or less rapidly, sometimes becoming very disabling.
Lipedema is in no way related to diet, to which it is falsely correlated.
Symptoms and diagnosis of lipedema
Lipedema mainly affects the legs (97% of cases). The increase in fat volume is accompanied by a fragility of the blood capillaries which release liquid into the surrounding tissues and are more sensitive to blows, resulting in bruising or hematoma.
This liquid released in the tissues is usually evacuated by the lymphatic system. However, in the long term, this permanent solicitation reduces the transport capacity of the lymphatic vessels, favouring the formation of edema, inflammation and subsequently collagen deposits, responsible for the irreversible fibrotization of the adipose tissue and the skin.
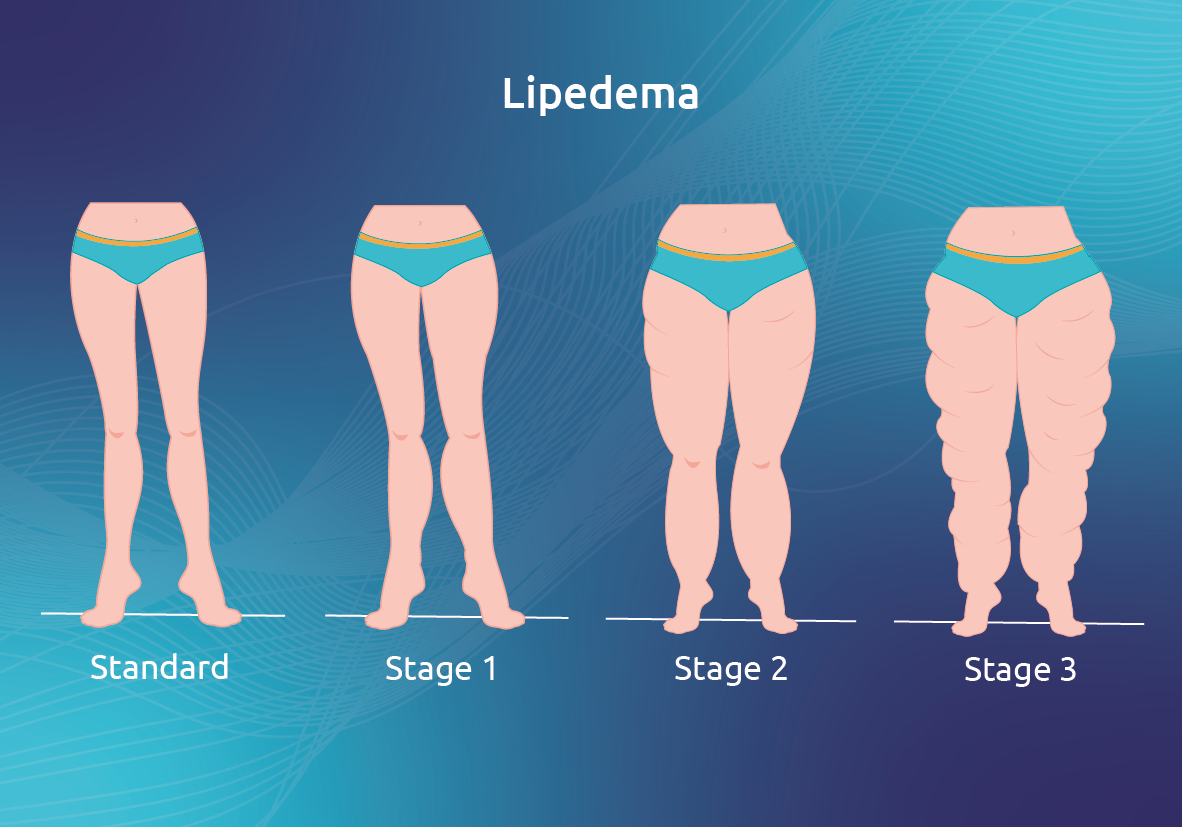
The diagnosis of lipedema can be established from different symptoms:
- non-harmonious distribution of fat from the hips to the ankles, which generates a pear-shaped silhouette
- fragility of the superficial microcirculation leading to small hematomas at the slightest impact
- superficial venous insufficiency with frequent varicose veins and stretch marks near the joints
- particular flexibility of the knee, ankle or elbow joints.
The diagnosis is essentially clinical but, in case of doubt, additional examinations may be necessary: CT scan, high resolution ultrasound, MRI and lymphoscintigraphy.
Treatment of lipedema
The treatments available are more or less effective depending on the stage of evolution of lipedema and the patient’s expectations. They must therefore be studied on a case-by-case basis, as the management of the condition is not codified (4).
Physiotherapy
- manual lymphatic drainage
- decongestive physiotherapy with short lengthening bands of less than 100%
- muscular exercises under multi-component bandages to release some of the sequestered water
Pressotherapy
- pressotherapy, pneumatic massage from distal to proximal with massage boots, as a complement to physiotherapy (2) (3). This technology can be used in the physiotherapist’s or vascular physician’s office, but also at home with a personal device.
Surgery(4)
- liposuction to reduce volume, reshape the trochanteric region and the inner thighs, with continuous elastic compression for the first 7 days, then only in the day for 4 to 6 weeks. The procedures can be repeated up to 6 times depending on the areas to be treated, with a minimum interval of one month between two liposuctions.
- skin resection of bulky masses located on the inner thighs or calves, with decongestive physiotherapy (low elasticity bandages) preoperatively to reduce the fluid component in order to facilitate wide resection, and postoperatively to stabilize the volume.
Complementary approaches
- wearing of custom-made class 2 or 3 elastic compression to maintain volume over the long term and act on venous insufficiency
- elevation of the limbs to reduce pain
- physical activity to maintain muscles and stabilize weight, especially in an aquatic environment to limit spontaneous superficial pain (aquagym, aquabike)
- skin care: hydration
- psychological care
Lipedema is aggravated by weight gain, yet it reacts only moderately to a restrictive diet and/or physical exercise; patients generally lose weight only in the “healthy” parts of the body.
The mechanisms of lipedema – identified in 1940 and since recognized as a chronic disease by the WHO (World Heath Organization) – are not yet well understood. Fortunately, research is advancing to provide better answers to patients and improve their quality of life.
- Langendoen SI, Habbema L, Nijsten TE, Neumann HA. Lipœdema : from clinical presentation to therapy. A review of the literature. Br J Dermatol 2009;161;980-6
- Szolnoky G, Varga M, Tuczai M, Dosa-Racz E, Kemeny L. Lymphedema treatment decreases pain intensity in lipedema. Lymphology 2011;44;178-82.
- Szolnoky G, Nagy N, Kovacs RK, Dosa-Racz E, Szabo A, Barsony K, et al. Complex decongestive physiotherapy decreases capillary fragility in lipedema. Lymphology 2008;41:161-6.
- S. Vignes – Unité de lymphologie, centre national de référence des maladies vasculaires rares, Hôpital Cognacq-Jay. Mise au point : lipœdème, une entité mal connue. Journal des Maladies Vasculaires 2012 ;37 ;213-218.